Abstract
Research Article
From Wallets to Waistlines: Exploring the Link between Family Income (Wage Distribution) and Obesity Indices in Pakistani Populations
Atif Akbar and Waqas Ghulam Hussain*
Published: 15 April, 2026 | Volume 10 - Issue 1 | Pages: 001-014
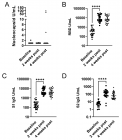
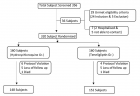
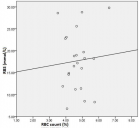
Obesity represents a significant public health challenge on a global scale, with its prevalence increasingly linked to socio-economic factors, most notably family income. This study investigates the relationship between family income and several obesity measures specifically, the Body Shape and Size Index (BSSI), Body Mass Index (BMI), Body Surface Area (BSA), Ponderal Index (PI), Weight/Body Mass (BM), and Height within a sample of 9,906 respondents from Pakistan. Utilizing descriptive statistics and p - values, the analysis aims to provide a comprehensive understanding of how variations in income affect these obesity indicators, ultimately informing potential public health interventions. The findings reveal a complex, variable association between family income levels and obesity measures that differs by the specific obesity index examined. For BSSI, individuals in the lowest income bracket demonstrated higher values (indicating greater adiposity), while for BMI and weight, higher income brackets showed elevated values. These mixed findings suggest that the direction of association depends critically on which obesity measure is analysed. The study reveals that lower-income families are more likely to face barriers in accessing nutritious food, engaging in physical activity, and achieving favourable health outcomes. This situation is often exacerbated by economic constraints that drive families toward caloric-dense, nutrient-poor food choices. The implications of this research are far-reaching, emphasizing the need for targeted public health strategies to address obesity, particularly among economically disadvantaged populations. The study advocates for policies that enhance food security, improve access to health-promoting resources, and create supportive environments for physical activity. Through a nuanced exploration of these relationships, the research aims to contribute valuable insights to the field of public health, promoting equity in health outcomes and addressing the root causes of obesity in Pakistan.
Read Full Article HTML DOI: 10.29328/journal.niogb.1001024 Cite this Article Read Full Article PDF
Keywords:
Obesity; Family income; Socio-economic factors; Body Mass Index (BMI); Health disparities; Nutritional access; Public health interventions
References
- Alam K. Global, regional, and national prevalence of child and adolescent overweight and obesity, 1990–2021, with forecasts to 2050: a forecasting study for the Global Burden of Disease Study. Lancet. 2025;405:785-812. Available from:https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(25)00397-6/fulltext
- Horta BL, Rollins N, Dias MS, Garcez V, Pérez-Escamilla R. Breastfeeding and later overweight or obesity: systematic review and meta-analysis. Acta Paediatr. 2023;112(1):34-41.
- Baidal JAW, Locks LM, Cheng ER, Blake-Lamb TL, Perkins ME, Taveras EM. Risk factors for childhood obesity in the first 1,000 days: a systematic review. Am J Prev Med. 2016;50(6):761-779.Available from: https://doi.org/10.1016/j.amepre.2015.11.012
- Buoncristiano M, Williams J, Simmonds P, Nurk E, Ahrens W, Nardone P, et al. Socioeconomic inequalities in overweight and obesity among 6- to 9-year-old children in 24 countries from the WHO European region. Obes Rev. 2021;22:e13213. Available from:https://doi.org/10.1111/obr.13213
- Eskandari F, Lake AA, Rose K, Butler M, O'Malley C. Influences of food environments and food insecurity on obesity in high-income countries: a mixed-method systematic review and meta-analysis. Food Sci Nutr. 2022;10(11):3689-3723.
- Anekwe CV, Jarrell AR, Townsend MJ, Gaudier GI, Hiserodt JM, Stanford FC. Socioeconomics of obesity. Curr Obes Rep. 2020;9:272-279. Available from:https://doi.org/10.1007/s13679-020-00398-7
- Anderson LN, Yoshida-Montezuma Y, Dewart N, Jalil E, Khattar J, De Rubeis V, et al. Obesity and weight change during the COVID-19 pandemic in children and adults: a systematic review and meta-analysis. Obes Rev. 2023;24(5):e13550. Available from:https://doi.org/10.1111/obr.13550
- Cai Q, Qian M, Chen M. Association between socioeconomic status and post-stroke depression in middle-aged and older adults: results from the China Health and Retirement Longitudinal Study. BMC Public Health. 2024;24(1):1007. Available from: https://doi.org/10.1186/s12889-024-18503-z
- Williams MS, McKinney SJ, Cheskin LJ. Social and structural determinants contributing to obesity disparities. Curr Obes Rep. 2024;13(3):617. Available from:https://doi.org/10.1007/s13679-024-00578-9
- Nagi MA, Ahmed H, Rezq MAA, Sangroongruangsri S, Chaikledkaew U, Almalki Z, et al. Economic costs of obesity: a systematic review. Int J Obes. 2024;48(1):33-43. Available from:https://doi.org/10.1038/s41366-023-01398-y
- Yang F, Katumba KR, Griffin S. Health inequality impact in economic evaluation in LMICs: a systematic review. Expert Rev Pharmacoecon Outcomes Res. 2022;22(1):17-25. Available from: https://doi.org/10.1080/14737167.2021.1954505
- Hassen HY, Bowyer M, Gibson L, Abrams S, Bastiaens H. Cardiovascular disease knowledge, risk perception and socioeconomic disparities among adults in vulnerable communities of Belgium and England. BMC Public Health. 2022;22(1):197. Available from:https://doi.org/10.1186/s12889-022-12608-z
- Bridger Staatz C, Kelly Y, Lacey RE, Blodgett JM, George A, Arnot M, et al. Socioeconomic position and body composition in childhood in high- and middle-income countries: a systematic review and narrative synthesis. Int J Obes. 2021;45(11):2316-2334. Available from:https://doi.org/10.1038/s41366-021-00899-y
- Snow MS. The invasion of Ukraine and the global food crisis of 2022: responding to food supply shocks. In: The Great Power Competition Volume 5. Springer Nature Switzerland; 2023. p. 351-387.
- Buszkiewicz JH, Hill HD, Otten JJ. Association of state minimum wage rates and health in working-age adults using the National Health Interview Survey. Am J Epidemiol. 2021;190(1):21-30. Available from: https://doi.org/10.1093/aje/kwaa018
- Theis DR, White M. Is obesity policy in England fit for purpose? Milbank Q. 2021;99(1):126-170. Available from: https://doi.org/10.1111/1468-0009.12498
- Opotow S. Subverting an ethical code: APA and the post-9/11 war on terror. Qual Psychol. 2022;9(3):344. Available from:https://psycnet.apa.org/record/2022-46148-001
- Azen R, Walker CM. Categorical data analysis for the behavioral and social sciences. Routledge; 2021. Available from:https://www.routledge.com/Categorical-Data-Analysis-for-the-Behavioral-and-Social-Sciences/Azen-Walker/p/book/9780367352769
- Privitera GJ. Research methods for the behavioral sciences. Sage Publications; 2024.
- Gilman J, Walls L, Bandiera L, Menolascina F. Statistical design of experiments for synthetic biology. ACS Synth Biol. 2021;10(1):1-18. Available from:https://doi.org/10.1021/acssynbio.0c00385
- Hallquist MN, Wright AG, Molenaar PCM. Problems with centrality measures in psychopathology symptom networks. Multivariate Behav Res. 2021;56(2):199-223. Available from: https://doi.org/10.1080/00273171.2019.1640103
- Ayenew LG, Hoelscher MA, Emshoff JG, Kidder DP, Ellis BA. Evaluation of the public health achievements made by projects supported by a federal contract mechanism at the Centers for Disease Control and Prevention (CDC), USA. Eval Program Plann. 2021;88:101949. Available from: https://doi.org/10.1016/j.evalprogplan.2021.101949
- Liu Y, Trude ACB, Song S, Jiang N, Wang S, Gittelsohn J, et al. Childhood obesity inequality in northeast China. BMC Public Health. 2023;23(1):318. Available from:https://doi.org/10.1186/s12889-023-15194-w
- Anderson LN, Fatima T, Shah B, Smith BT, Fuller AE, Borkhoff CM, et al. Income and neighbourhood deprivation in relation to obesity in urban dwelling children 0–12 years of age: a cross-sectional study from 2013 to 2019. J Epidemiol Community Health. 2022;76(3):274-280. Available from: https://doi.org/10.1136/jech-2021-216455
- Gómez G, Kovalskys I, Leme ACB, Quesada D, Rigotti A, Cortes Sanabria LY, et al. Socioeconomic status impact on diet quality and body mass index in eight Latin American countries: ELANS study results. Nutrients. 2021;13(7):2404. Available from: https://doi.org/10.3390/nu13072404
- Green H, Fernandez R, MacPhail C. Social determinants of health and health outcomes among adults during the COVID-19 pandemic: a systematic review. Public Health Nurs. 2021;38(6):942-952. Available from: https://doi.org/10.1111/phn.12959
- Bubach S, Horta BL, Gonçalves H, Assunção MCF. Early age at menarche and metabolic cardiovascular risk factors: mediation by body composition in adulthood. Sci Rep. 2021;11(1):148. Available from: https://doi.org/10.1038/s41598-020-80496-7
- Ayuningtyas D, Hapsari D, Rachmalina R, Amir V, Rachmawati R, Kusuma D. Geographic and socioeconomic disparity in child undernutrition across 514 districts in Indonesia. Nutrients. 2022;14(4):843. Available from: https://doi.org/10.3390/nu14040843
- Gao M, Wells JC, Johnson W, Li L. Socio-economic disparities in child-to-adolescent growth trajectories in China: findings from the China Health and Nutrition Survey 1991–2015. Lancet Reg Health West Pac. 2022;21. Available from:https://doi.org/10.1016/j.lanwpc.2022.100399
- Mekonnen T, Papadopoulou E, Arah OA, Brantsæter AL, Lien N, Gebremariam MK. Socioeconomic inequalities in children’s BMI trajectories in Norway. Sci Rep. 2021;11(1):4979. Available from: https://doi.org/10.1038/s41598-021-84615-w
- Victora CG, Christian P, Vidaletti LP, Gatica-Domínguez G, Menon P, Black RE. Maternal and child undernutrition in LMICs. Lancet. 2021;397(10282):1388-1399.
- Victora CG, Christian P, Vidaletti LP, Gatica-Domínguez G, Menon P, Black RE. Maternal and child undernutrition in LMICs. Lancet. 2021;397(10282):1388-1399.
- Udalova V, Bhatia V, Polyakova M. Association of family income with morbidity and mortality among US lower-income children and adolescents. JAMA. 2022;328(24):2422-2430. Available from: https://doi.org/10.1001/jama.2022.22778
- Shebanina E, Burkovska A, Lunkina T. Global aspects of food security in the world: economic dimensions. 2023. Available from: https://doi.org/10.31521/modecon.v38%282023%29-27
- Power M. Revising perspectives on neoliberalism, hunger and food insecurity. In: Hunger, Whiteness and Religion in Neoliberal Britain. Policy Press; 2022. p. 18-36.
- Kumar P, Srivastava S, Chauhan S, Patel R, Marbaniang SP, Dhillon P. Socio-economic inequality in thinness and stunting among adolescents in Uttar Pradesh and Bihar, India. PLoS One. 2021;16(2):e0247526. Available from: https://doi.org/10.1371/journal.pone.0247526
- Kåks P, Målqvist M, Forsberg H, Fjellborg AA. Neighborhood income inequality, maternal deprivation and neonatal health in Sweden. SSM Popul Health. 2025;29:101745. Available from: https://www.sciencedirect.com/science/article/pii/S2352827324001460
- Malovic P, Bjelica D. Impact of socioeconomic status on obesity of adolescents. Iran J Public Health. 2021;50(11):2337. Available from: https://doi.org/10.18502/ijph.v50i11.7591
- Galvan MC, Pyrczak F. Writing empirical research reports: a basic guide for students of the social and behavioral sciences. Routledge; 2023.
- Wang K, Wu C, Yao Y, Zhang S, Xie Y, Shi K, Yuan Z. Socio-economic factors and obesity risk among Chinese adults. Glob Health Res Policy. 2022;7(1):41. Available from: U8--https://doi.org/10.1186/s41256-022-00274-y
Figures:
Similar Articles
-
The interaction between photonic technology and physical exercise: The action of low-level laser therapyAntonio Eduardo de Aquino Jr*,Fernanda Mansano Carbinatto. The interaction between photonic technology and physical exercise: The action of low-level laser therapy. . 2017 doi: 10.29328/journal.hodms.1001003; 1: 010-013
-
Behavioral factors of Abdominal Obesity and effects of lifestyle changes with Fiber AdequacyRoberto Carlos Burini*,Hugo Tadashi Kano,Mariana Santoro Nakagaki,Patricia Baston Frenhani,Katia Cristina Portero-McLellan. Behavioral factors of Abdominal Obesity and effects of lifestyle changes with Fiber Adequacy. . 2017 doi: 10.29328/journal.hodms.1001004; 1: 014-022
-
Upper gut bacterial overgrowth is a potential mechanism for Glucose Malabsorption after Vertical Sleeve GastrectomyTimothy R Koch*,Timothy R Shope,Matthew E Sharbaugh. Upper gut bacterial overgrowth is a potential mechanism for Glucose Malabsorption after Vertical Sleeve Gastrectomy. . 2017 doi: 10.29328/journal.hodms.1001006; 1: 030-035
-
Body mass index in a group of security forces (policemen). Cross-sectional studyGuillermo Padrón Arredondo*. Body mass index in a group of security forces (policemen). Cross-sectional study. . 2018 doi: 10.29328/journal.niogb.1001007; 2: 001-004
-
Herbal approach for obesity managementPreeti Singh*. Herbal approach for obesity management. . 2018 doi: 10.29328/journal.niogb.1001008; 2: 005-016
-
Dietary and Lifestyles assessment among Obese Women in Gaza City, PalestineMarwan O Jalambo*,Basil Kanoa,Mohammed S Ellulu,Smaher Younis,Mueen El-Kariri. Dietary and Lifestyles assessment among Obese Women in Gaza City, Palestine. . 2018 doi: 10.29328/journal.niogb.1001009; 2: 017-025
-
Obesity-Treatment by drugsSahithi G*. Obesity-Treatment by drugs. . 2019 doi: 10.29328/journal.niogb.1001010; 3: 001-001
-
ECHO…for a change!!Manish Motwani*,Rajeev Palvia,Bhavesh Nanda,Mahek Motwani,Bhakti Chaubal,Jyoti Kesarkar, Bhakti Mange,Sneha Shukla. ECHO…for a change!!. . 2020 doi: 10.29328/journal.niogb.1001011; 4: 001-003
-
Obesity Surgery in SpainAniceto Baltasar*. Obesity Surgery in Spain. . 2020 doi: 10.29328/journal.niogb.1001013; 4: 013-021
-
The review of the relationship between UCP2 and obesity: Focusing on inflammatory-obesityMohamadreza Alivand*,Beitullah Alipour*,Sara Moradi,Yaser Khaje-Bishak,Maedeh Alipour. The review of the relationship between UCP2 and obesity: Focusing on inflammatory-obesity. . 2021 doi: 10.29328/journal.niogb.1001015; 5: 001-013
Recently Viewed
-
The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain SyndromeMohammed Amine Elafari*,Mohammed Amine Bibat,Mamad Ayoub,Amine Slaoui,Tarik Karmouni,Abdelatif Koutani,Khalid Elkhader. The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain Syndrome. Int J Clin Microbiol Biochem Technol. 2026: doi: 10.29328/journal.ijcmbt.1001036; 9: 022-026
-
One-time CRISPR Adenine Base Editing Intervention in SMA: From SMN2 Splice Correction to Motor Neuron RescueSheena P Kochumon,Najma Nujoom,Prem Jagadeesan,Vinod Scaria,DM Vasudevan,KP Soman,Cherupally Krishnan Krishnan Nair*. One-time CRISPR Adenine Base Editing Intervention in SMA: From SMN2 Splice Correction to Motor Neuron Rescue. J Genet Med Gene Ther. 2026: doi: 10.29328/journal.jgmgt.1001014; 9: 1-6
-
The Role of Genetic Mutations in the HPGD & SLCO2A1 Genes in Pachydermoperiostosis SyndromeShahin Asadi*,Arezo Zare,Sima Koohestani. The Role of Genetic Mutations in the HPGD & SLCO2A1 Genes in Pachydermoperiostosis Syndrome. J Genet Med Gene Ther. 2025: doi: 10.29328/journal.jgmgt.1001013; 8: 001-005
-
Adult Bladder Exstrophy with Premalignant Changes Following Failed Reconstruction: A Case ReportMohammed Amine Elafari*,Mamad Ayoub,Mohamed Amine Zaki,Mohammed Amine Bibat,Amine Slaoui,Tarik Karmouni,Abdelatif Koutani,Khalid Elkhader. Adult Bladder Exstrophy with Premalignant Changes Following Failed Reconstruction: A Case Report. J Clin Med Exp Images. 2026: doi: 10.29328/journal.jcmei.1001044; 10: 020-023
-
Low Level Light Therapy (LLLT): Penetration and PhotobiomodulationCecilia Young*,Cheuk Lam Mak. Low Level Light Therapy (LLLT): Penetration and Photobiomodulation. J Oral Health Craniofac Sci. 2017: doi: 10.29328/journal.johcs.1001015; 2: 080-082
Most Viewed
-
Physical Performance in the Overweight/Obesity Children Evaluation and RehabilitationCristina Popescu, Mircea-Sebastian Șerbănescu, Gigi Calin*, Magdalena Rodica Trăistaru. Physical Performance in the Overweight/Obesity Children Evaluation and Rehabilitation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001030; 8: 004-012
-
Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging PresentationKarthik Baburaj*, Priya Thottiyil Nair, Abeed Hussain, Vimal MV. Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging Presentation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001029; 8: 001-003
-
Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trialSathit Niramitmahapanya*,Preeyapat Chattieng,Tiersidh Nasomphan,Korbtham Sathirakul. Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trial. Ann Clin Endocrinol Metabol. 2023 doi: 10.29328/journal.acem.1001026; 7: 00-007
-
Exceptional cancer responders: A zone-to-goDaniel Gandia,Cecilia Suárez*. Exceptional cancer responders: A zone-to-go. Arch Cancer Sci Ther. 2023 doi: 10.29328/journal.acst.1001033; 7: 001-002
-
Ectopic adrenal tissue at the spermatic cordAbdallah Chaachou,Nizar Cherni,Wael Ferjaoui*,Mohamed Dridi,Samir Ghozzi. Ectopic adrenal tissue at the spermatic cord. J Clin Med Exp Images. 2022 doi: 10.29328/journal.jcmei.1001024; 6: 001-002

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."